Quick Email Now!
-
-
Call Us Today !
+91 9646350900
Quick Email Now!
Call Us Today !
We Provide Each Patient With The Highest Possible Level Of Care

Many diseases of the urinary tract require endoscopic surgery. These include kidney stones, ureteric stones, prostate, urinary bladder stones, bladder tumours, ureteral strictures, ureteral tumours and blockage in the kidney due to various reasons. Usually we divide urinary tract into two parts namely lower tract (urethra, urinary bladder) and upper tract (kidney and ureter).
There are two main approaches to endoscopic surgery. The first approach is from a “retrograde” fashion means through urethra under general or regional anaesthesia. Using a fiberoptic scope (ureteroscope) connected to a camera, the surgeon watches a television monitor as the scope is inserted into the bladder, then advanced into one of the ureters and then into the kidney depending upon the location of the stone or other pathology, under fluoroscopy to guide the course. Often, the surgeon may use laser to break up stones or remove prostate.
Postoperative recovery depends on the disease process. Most of the time the patients are discharged within 24 - 48 hours if they do not have a fever, and are able to take liquids and normal diet orally following surgery.
The second approach is from the “antegrade”, or “percutaneous” fashion. This means to approach the kidney through the skin from the back under general or regional anaesthesia.
With the help of fluoroscopy or real time x-ray an access to the affected kidney is obtained by puncturing the renal calyces through skin. This is the most important and crucial step because wrong puncture can result in excessive bleeding during tract dilation. A guidewire is placed into the kidney and then the tract is serially dilated with dilator. Depending upon the size of stones the tract is dilated. In Mini PCNL, most commonly done now a days even for larger stones, tract is dilated only up to 15 to 19.5 F. For regular PCNL dilation up to 26 F is sufficient for removing even large staghorn stones. Lesser the diameter of the tract lower is the chance bleeding. After dilating tract, we place the nephroscope, and with the help of pneumatic or ultrasound lithoclast (in case of regular PCNL) or laser (in case of Mini PCNL) kidney stones are removed. Often the urologist will leave a tube in the kidney to drain the urine, and any clots or stone dust. Within the next 24 hours an x-ray is taken. If there is no residual stone fragment then nephrostomy tube is taken out and the patient is discharged home. Occasionally there may be a urine leak from the entry wound which usually settles in few hours.
Bladder cancer: Blood in urine, frequency and urgency
Kidney cancer: Often diagnosed early on imaging of the abdomen done other reasons such as routine health check-up. Sometimes blood in urine, flank pain seen in late course.
Prostate cancer: Often diagnosed early on imaging of the abdomen done other reasons such as routine health check-up. Sometimes blood in urine, flank pain seen in late course.
Prostate cancer is a common cancer in men. Early cancer may not cause any symptoms or the symptoms may be similar to those in a man with benign prostatic hypertrophy (BPH). Hence, the only way to diagnose this disease early is by getting an evaluation by a urologist. Digital rectal examination and a blood test known as serum PSA or prostate specific antigen may indicate the need for biopsy (histopathological examination prostatic tissue obtained by trans rectal ultrasound guided needle core biopsy). Biopsy is carried out by the urologist or radiologist under local anaesthesia on OPD basis. Men with confirmed cancer may need surgery, radiation therapy or medication depending upon stage of the disease. Radical prostatectomy is done for men with early cancer prostate who are otherwise fit and have life expectancy of 15 years.
Bladder tumor is an important cause of blood in the urine after 40 years of age. Gross, painless hematuria is the primary symptom in 85% of patients with a newly diagnosed bladder tumor, and microscopic hematuria (red blood cells seen under microscope during routine examination of urine) occurs in virtually all patients more commonly seen in smokers. Most tumors are cancerous and are a form of urothelial carcinoma (previously known as transitional cell carcinoma). Because urothelial cancer is a cancer of the environment and age, the incidence and prevalence rates increase with age, peaking in the eighth decade of life, and there is a strong association between environmental toxins and urothelial cancer formation. Males are 3 to 4 times more likely to develop bladder cancer than females, presumably because of an increased prevalence of smoking and exposure to environmental toxins. These cancers can be classified as invasive or non-invasive, depending on whether they have involved the bladder muscle layer. Tumors that are non-invasive are less likely to become life-threatening but may need careful follow up since they have a strong tendency to recur. Tumors that invade muscle need more aggressive treatments such as bladder removal (radical cystectomy), radiation therapy with or without chemotherapy depending upon local staging. Radical cystectomy is the gold standard treatment for muscle invasive bladder cancer.


A kidney stone up to the size 15 - 20 mm can be removed through latest technique without puncturing the kidney known as RIRS (Retrograde Intra Renal Surgery). This is done with the help of flexible ureteroscope passed through urethra into the ureter then into kidney under general anaesthesia. Stone in the kidney is fragmented into dust with laser and flushed out with irrigation fluid. A DJ stent is placed and removed after 3-4 weeks after no significant residual fragment confirmed with sonography or plain CT KUB.

The patient should expect to resume their normal activities within 7-10 days following ureteroscopic surgery, 10-14 days following percutaneous surgery (Mini or regular PCNL) and 2-3 days following RIRS.
Know your prostate?
The prostate is part of male reproductive system. It is a walnut-sized gland and is found only in men. It is located just below the urinary bladder and surrounds the proximal urethra (tube along the penis that takes urine out of the body from the urinary bladder). Prostate produces nutrients for the sperm and an enzyme which liquefies the semen that helps in fertilization and thus in reproduction.
The gland is divided into three zones, peripheral, transitional and central. In Benign Prostatic Hyperplasia (BPH), there is an overgrowth of cells in the central portion of the prostate. This constricts the urethra, reduces the flow of urine and makes it difficult for the patient to empty his bladder.
BPH is very common, affecting about one third of men over 50.
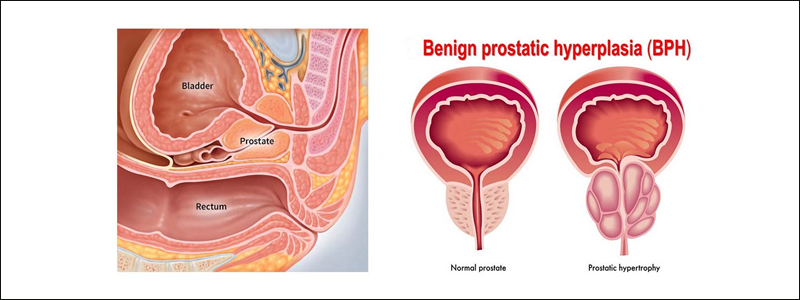
As men get older, some physiological changes occur in our body like hair becomes sparse and grey, skin becomes wrinkled the same way the cells of prostate begin to increase in number, which increases the size of the prostate. This is called benign prostatic hyperplasia (BPH), which means extra growth of normal (non-cancerous) cells. Usually this is not serious, but sometimes the prostate grows so large that it puts pressure on the urethra (the tube through which you pass urine).
You may find difficulty in passing urine and may notice other urinary symptoms such as:
Weak urinary stream
strain to pass urine
not able to empty your bladder completely
need to go to the toilet more often (known as frequency)
Urgency (difficult to postpone urination)
Urgency leakage of urine
Nocturia (to get up at night from sleep to pass urine more than once)
Because of the squeezing effect on your urethra, you may have to use a lot of pressure to pass urine. In the long term, this can damage your bladder and kidneys. This also sometime can cause kidney failure
Many of the patients who is symptomatic due to enlarged prostate can be treated with medicines, but only few of the patients require surgical treatment (HoLEP)
Definitive indication for surgical treatment:
Recurrent refractory urinary retention (patient on medical treatment develops retention of urine).
Failure of medical treatment
Recurrent urinary tract infection.
Bladder stones with enlarged prostate.
Renal Failure due to backpressure on the urinary bladder and kidney.
Recurrent gross haematuria (repeated blood in urine) due to prostatic enlargement.
Not everyone who has an enlarged prostate will need treatment. However, your urologist has recommended holmium laser treatment as the best option to relieve your symptoms. It will make it easier for you to pass urine and may relieve your other symptoms. If you do not take treatment, your prostate will continue to grow. This may make your symptoms worse and increases the possibility of problems with your bladder and/or kidneys.
This surgery is done under regional (spinal) or general anaesthesia. A thin long instrument fitted with telescope is inserted into the urethra. The high-powered holmium laser fibre is then inserted through this instrument and used to carefully remove the prostatic tissue (adenoma which is causing obstruction to the urethra, the same way you remove orange pulp from its peel).
The prostatic tissue removed by holep can be examined under microscope by histopathologist to check for cancerous cells. The prostatic tissue, removed by some other laser procedures, is not suitable for microscopic examination.
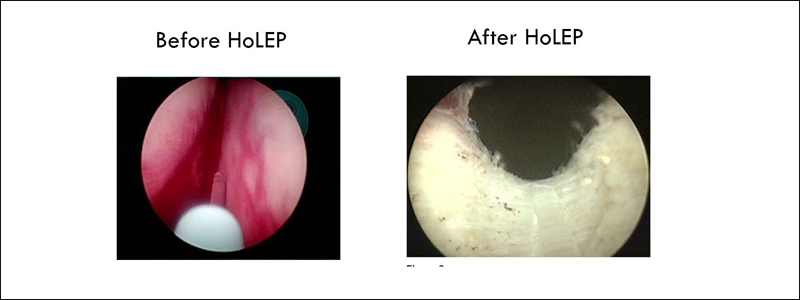
The holmium laser seals the blood vessels of the prostate tissue. This means there is very little blood loss in comparison to the other surgical options outlined below.
Holep is very safe for cardiac patient who are on blood thinner like Ecosprin, has pacemaker or low pumping capacity of the heart.
Prostate size is not a limit for holep, any big size prostate can be removed endoscopically without major complications as compared to other surgical methods. Re-operation rate is very minimal as compared to TURP and other laser procedure.
The catheter that is inserted after the procedure can usually be removed between 24 - 48 hours of the surgery. This allows you to leave hospital more quickly than the other surgical options below and reduces your recovery time.
There are several alternative treatment options outlined below, although they may not all be appropriate for you. Your urologist will discuss these with you if they are suitable for your situation:
Medicines:Medicines. There are two types of medicine available. They either shrink the prostate, or relax the prostatic muscle and bladder neck to improve the flow of urine. However, the effects only last as long as you take the medicine
Transurethral resection of the prostate (TURP): This is a endoscopic surgery to remove the parts of prostate in piecemeal that are causing obstruction to the flow of urine.
Open surgery (Millin’s prostatectomy, Freyer’s prostatectomy). This is considered if the prostate is too large to be removed by TURP.
Prostatic stent Prostate stent is an option for only selected patients who are very high risk and not fit for TURP (transurethral resection of the prostate). This is where an expandable tube made up of thin metal or plastic interwoven wire is inserted into the urethra, to widen the prostatic urethra. The long term results are not satisfactory.
Prostatic urethral lift (PUL): Prostatic urethral lift is also an endoscopic procedure. The urolift system is like H shaped device comprising of two metallic steel arms with nylon suture bridge. The implant device is designed to retract the prostate to allow to open the prostatic urethra. The implants are retained in the prostate to maintain an expanded urethral lumen. This method is not yet well established.
Prostate arterial embolization: This is a minimally invasive procedure that blocks the arteries which supply blood to the prostate, and is performed under local anaesthetic. This method is still under trial.
Urinary frequency and urgency:These are transient symptoms after holep should go within four to six weeks.
Transient SUI (stress urinary incontinence): Nearly 90 % of the men who had transient stress urinary incontinence achieves complete resolution within 4-6 weeks.
Urinary infection: This can cause symptoms such as pain during micturition and blood in the urine. This happens to about five in 100 patients and is transient. This can be very easily treated as advised by your urologist
Retrograde ejaculation:Semen goes into bladder when you ejaculate and comes out when you pass urine. This is not harmful. This does not affect your sexual life and orgasm, but your fertility may be affected.
Erectile dysfunction: The nerves that control your erections are very close to the prostate gland. About 15 in 100 patients may notice a slight deterioration in the quality of their erections, which will usually respond to medication. However, about three in 10 men will notice that their erectile function improves significantly because their quality of life has improved after surgery.
Bleeding: There is much less bleeding with holmium laser treatment compared with other surgical procedures for an enlarged prostate. If the bleeding is severe you may need a blood transfusion, but this is extremely rare.
Prostate re-growth: Very rare with holep as compared to other modalities.
Stricture urethra: This reduces the flow of urine. This happens to about two in 100 men who have this procedure. Which is very easily manageable with minor endoscopic surgery called EIU.
Your urologist will discuss with you about the details of the surgery and its course and complications.
After proper evaluation by your urologist you will be advised to attend the pre-assessment clinic where anaesthetist will assess your suitability for surgery under anaesthesia.
If you smoke, you may be asked to stop smoking, as it increases the risk of developing a chest infection or DVT. Smoking can also delay wound healing because it reduces the amount of oxygen that reaches the tissues in your body.
Please do not eat or drink anything for six hours before your planned time of surgery. You are allowed to drink water only up to two hours before your surgery. If you continue to eat or drink after this, your surgery will be cancelled.
Please continue to take all your medicines unless you are told otherwise and remember to bring them into hospital with you.
WHAT SHOULD I EXPECT WHEN I COME TO HOSPITAL?
If you arrive on the ward the day before your surgery, you will be seen by a nurse who will ask you few basic questions, show you around the ward and prepare you for theatre.
PRE-OPERATIVE CONSENT
We want to involve you in all the decisions about your care and treatment. If you decide to go ahead, you will be asked to sign a consent form by your consultant or one of his team to confirm that you agree to have the procedure and understand what it involves.
AFTER HOLEP (IMMEDIATE POST OP IN THE WARD)
Usually patient does not have any pain from the operation, but you may have some discomfort due to the catheter. Some men experience bladder spasms (contractions) caused by the catheter rubbing against the trigone (lower part of the bladder) inside your bladder. The spasms result in urine passing down the sides of the catheter which may leak into your underwear. The spasms may also make you have the urge to pass urine, which can be uncomfortable. If you experience these spasms or have a sudden urge to pass urine, please tell your nurse/urologist, as these symptoms can often be relieved with simple medicine.
WHAT PROBLEMS MIGHT BE EXPERIENCED AFTER THE SURGERY?
You may experience a mild burning or find it a little uncomfortable to pass urine initially. This is because your prostatic urethra will be swollen and sore from the surgery and having the catheter in place. This is normal and usually does not last long (not more than 10 – 14 days).
You may notice some blood either before or after passing urine which will resolve after 7 - 10 days, although this is much less common with holep.
You will be advised not to strain during defaecation and not travel on bike or scooter which can cause blood in urine.
Some men find that they cannot pass urine when the catheter has been removed, but not to worry at all this is transient. If this happens, a new catheter but of smaller calibre will be inserted into your urethra and you may need to keep this in for few days to allow your bladder to rest.
It is common to have some difficulty to postpone urination (urinary urgency) for short time following surgery which usually subsides in 2-3 weeks. You may have less control in passing urine for a short time after surgery. If you experience this, please tell your doctor, who will teach you pelvic floor exercises to improve your urinary control.
WHEN TO COME FOR FOLLOW-UP?
You should come after 4 weeks for follow up after surgery with your biopsy report or earlier if you face any problems. You will be asked to pass urine into a special machine (flow rate machine) to assess your urinary flow after your treatment, so you will need to attend the clinic with a full bladder. You will have a scan of your bladder to make sure you are emptying your bladder completely when you pass urine.
WHEN CAN I GO BACK TO MY NORMAL ACTIVITIES?
Heavy lifting: Do not lift anything heavy until one week after your surgery.
Sex: You should be able to have sexual intercourse soon after surgery, as long as there is no bleeding and you and your partner both feel ready.
Driving: You must ask someone to take you home as you are not allowed to drive within 24 - 48 hours of having an anaesthetic. You should only drive again when you are free of pain and able to perform an emergency stop comfortably.
Diet:Same as you were eating before surgery.
Heavy lifting: Do not lift anything heavy until one week after your surgery.